- Medical Matters
PCOS and Sleep Disorders
by Tracey Parnell, MD
Polycystic ovarian syndrome is one of the most common hormone problems affecting women. Varying studies report PCOS in 5-30% of the females in reproductive years. In addition, up to 70% of cases may be under diagnosed.
By the Rotterdam Criteria, PCOS is diagnosed if two of the following three criteria are met:
1) oligomenorrhea (nine or fewer menses per year) or amenorrhea (no menses for a year)
2) Evidence of hyperandrogenism—increased testosterone by blood work or clinical signs of increased facial hair, male pattern hair loss, increased acne
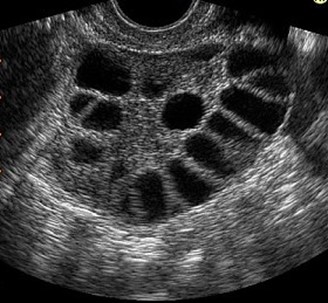
3) Multiple ovarian cysts by ultrasound
Part of the problem with PCOS is insulin resistance, which can affect the ovary as well as many body systems. Insulin resistance can lead to elevated androgens (male hormones like testosterone), which can lead to disrupted early follicle development, impaired ovulation and infertility. Women with PCOS are at increased risk of high blood pressure, elevated cholesterol, and heart disease, in addition to reproductive cancers, like endometrial cancer. They are also more likely to have obstructive sleep apnea (OSA), which is a sleep disorder caused by the airway collapsing during sleep, causing more disrupted, unrefreshing sleep. In one study by Vgontzas, et al, women with PCOS were thirty times more likely to have sleep apnea than controls (Odds ratio=30.6, 95% CI 7.2-139.4). Insulin resistance is a stronger risk factor than body mass index for developing sleep apnea. Yes, a woman can be thin and have both PCOS and OSA!
In a study by Tasali, PCOS women with OSA were more insulin resistant than those without OSA (adjusted odds ratio 7.1; 95% confidence interval, 1.7-45.7; P = 0.01). The higher the severity of OSA, the higher the insulin resistance.
Insulin resistance is also increased in women with limited or fragmented sleep. Clinically significant insomnia was found in 12.6% of women with PCOS.
When sleep quality is improved, such as when women with obstructive sleep apnea are treated with CPAP, the insulin resistance improves.
Women with PCOS can have difficulty achieving and maintaining a pregnancy. If they also have sleep apnea, their pregnancy may be at higher risk. Various studies have shown an increased risk of high blood pressure, intrauterine growth retardation, preeclampsia, and pre-term birth in women with OSA in pregnancy.
A recent study showed pregnant women with OSA have lower than normal progesterone levels tested in the first and second trimester. Perhaps the oxygen drops and disturbed sleep of OSA negatively affects the ability of the placenta to produce progesterone, but it could also be that the lower progesterone leads to less stimulation to breathe at night.
So, what can women do to improve their sleep if they have PCOS? If they snore, have been witnessed to stop breathing, or struggle to breathe in their sleep, or if they feel more sleepy than normal, they should talk to their doctor about being tested for sleep apnea. In the meantime, sleeping on the sides, aiming for ideal body weight, and addressing allergies/nasal congestion will help minimize the airway blockages of sleep apnea. For difficulty with insomnia, working on making the bedroom dark, cool and quiet, with regular bedtimes, and no electronics or bright light before bedtime can be a good start. Bright light in the morning is also helpful, with adequate exercise.
Oftentimes as women’s sleep improves, they will see their cycles improve. Women with severe OSA will often have heavy menses, and these will lighten when the sleep apnea is treated. Patients who chart their cycles will observe significant improvements in their chart, corresponding with improved sleep quality following treatment for sleep apnea.
In summary, sleep disorders, especially OSA, are common in PCOS, and can have serious health consequences. If you, or someone you know, has PCOS, make sure to ask for a sleep disorder evaluation and use cycle charting to observe improvements as treatment commences.
Vgontzas AN1, Legro RS, Bixler EO, Grayev A, Kales A, Chrousos GP 2001 Polycystic ovary syndrome is associated with obstructive sleep apnea and daytime sleepiness: role of insulin resistance. J Clin Endocrinol Metab. Feb;86(2):517-20
Tasali E1, Van Cauter E, Hoffman L, Ehrmann DA Impact of obstructive sleep apnea on insulin resistance and glucose tolerance in women with polycystic ovary syndrome. J Clin Endocrinol Metab. 2008 Oct;93(10):3878-84
Chen Y-H, Kang J-H, Lin C-C, et al. Obstructive sleep apnea and the risk of adverse pregnancy outcomes. Am J Obstet Gynecol 2012;206:136.e1-5
Sleep disturbances in women with polycystic ovary syndrome G Franik, et al. Gynecological Endocrinology, 27 June 2016
About The Author